In the previous parts (1, 2, 3, and 4) of this series, I have tried to illustrate potential explanations for why physicians are unable to see medical injuries and that they will frequently gaslight patients through their denial that these injuries could have occurred. The ideas I put forward only represent my best attempt to provide a hypothesis that could explain the observations I have made throughout my medical career. It is very likely in the future that my perspectives on these issues will change. I invite any critical feedback that will better elucidate a model that explains medical blindness and likewise feedback, particularly from other health care providers, on my proposed solutions to medical blindness.
When I speak with individuals who have been gaslighted by the medical field, their experiences often remind me of a lyric from a heavy metal song I heard on the radio about someone being told they will repent for the sins they had committed in life. I normally don’t listen to this genre and I was undecided if I should include it in the article, but I feel the need to quote this song as the way it is sung represents the best depiction I have found of the medical gaslighting experience.
The song can be listened to here, specifically at this time. The original version of the song (more pleasant) can be listened to here, specifically at this time
The relevant lyrics are as follows:
“Hear no evil
Don’t see no evil
Don’t you lay no evil down on me
You’re going to burn in h***
Speak no evil
Don’t you think no evil
Don’t you play with evil
Cause I’m free”
Often when someone attempts to present the occurrence of a medical injury to a doctor, as described in the above lyrics, they are met with aggressive denial not that different from the experience a heretic would face when speaking blasphemy to those in power during the Middle Ages. Since Allopathic Medicine has positioned itself as the religious institution of our era, it helps to explain why the same experience is repeated; challenging the sanctity of Western Medicine is not unlike denying a religion’s declaration of God.
Being someone who challenges the dogma of Allopathic Medicine in order to have a life-altering adverse event recognized is a difficult experience no matter how you slice it. Most of the medical field has trouble being able to see the injury, many doctors don’t even want to believe it could have happened, and almost everyone seems to be ready to gaslight you into believing the adverse event never occurred, often without even realizing that is truly a horrible thing to do to a patient.
In most cases when people are being difficult and refusing to hear a different point of view, you can just accept your differences and not engage with them. However, in this case as an injured patient, you often you have no choice but to press the issue because your livelihood depends on the adverse event being acknowledged. To have success in this endeavor, I believe 5 areas need to be focused on:
1. Understanding where the doctor is coming from, and being able to see things from their perspective.
2. Understanding the framework they operate within and what they are able to do within it.
3. Knowing how to present yourself to the doctor so you will be listened to.
4. Knowing what to ask for and how to communicate with the doctor.
5. Knowing how to find the right doctor.
Where is the Doctor coming from?
In this series so far, I’ve attempted to explain where doctors are coming from when they see medical injuries that they turn a blind eye to. The primary issues I’ve focused on are as follows:
•The human body is very complicated, and people typically need models that simplify that complexity to understand what is occurring.
•Doctors often will not see something unless they are taught to look for it, and it is rare for that they are trained to recognize iatrogenic (i.e. pharmaceutically induced) adverse reactions.
•Medical training is an arduous experience that creates a faith in the practice and a psychological investment in believing the medical “truths” you learned are infallible and superior to all other “truths.”
•No one wants to believe they hurt a patient, so they will often lie to themselves to deny that an injury happened.
•The corporatized practice of medicine forces most doctors to spend very short periods of time with patients where they are only able to scratch at the surface of the complex issues in each patient.
I would like to discuss a historical example and a patient experience to further illustrate these points:
1. A complaint I have heard raised across the internet in the last year is that very few doctors even know what VAERS is, and as a result the adverse events from the vaccinations are never reported. This is not a new issue; for decades I have heard the same story from parents of vaccine injured children.
In American medical education, beyond what is deemed necessary to produce the basic competency to be a practicing physician, most of what is taught is reflective of what will be tested on medical board examinations as “boards are everything” and the quality of each medical school is largely determined by the board scores of its students. As you might imagine, this allows a significant influence to be exerted on the medical education process by having the medical boards emphasize pharmaceutical interventions and de-emphasize iatrogenesis.
Of note, I have heard from a lot of people over the years that pharmaceutical companies have bought out the organizations responsible for producing board examinations, but while the tests are reflective of an industry bias, I have not been able to establish systemic bribery by Big Pharma occurs that shapes the structure of medical board examinations.
The board examinations for medical students do test medical ethics and certain governmental laws pertaining to the practice of medicine. However, most of this knowledge is learned during post-graduate medical education (medical residency), as this knowledge is emphasized on later board examinations and within federally required training modules at the hospital(s) the medical resident trains within.
In the late 1980s, so many people were being injured by the older DTP vaccine (which not long after was pulled from the USA market and now just kills children in Africa) that the legal costs of its vaccine injuries were threatening to bankrupt the vaccine manufacturer. Two fundamental issues existed at the time: the difficulty of vaccine injured parents getting financial compensation for their children’s injury in court (it was a long and arduous process), and the US government being at risk of losing its vaccine program due to the manufacturers paying more in court settlements than they were making from their vaccinations.
Fauci brokered a deal President Reagan accepted that transferred liability away from the vaccine manufacturers and onto the federal government. To do so, a parallel legal system was created within the Department of Health and Human Services, which was intended to make it much easier for parents of vaccine injured children to earn compensation and not go through the horrendous process they had experienced within the regular court system.
Prior to COVID, National Childhood Vaccine Injury Act of 1986 was probably the most damaging health care policy in US history. The 1986 act incentivized pharmaceutical companies to start producing large numbers of unsafe vaccines (as they no longer had any liability) which were then given to the millennial (and subsequent) generation, creating the sickest generations in American history . At the same time the manufacturer’s liability was removed, Fauci sold out the American people and turned the NIH (and CDC) into pharmaceutical product pipelines (discussed here and here). This policy change likewise triggered a proliferation of the number of required pediatric vaccinations (you can compare before and after 1986 here) and an epidemic of neurological and autoimmune conditions within the population followed not long after.
One of the major problems with the 1986 act was that contrary to what had been promised, it became very difficult to be compensated in the special court for a vaccine injury. This was problematic as the vaccine court became only place you could go as the regular liability the vaccine manufacturers had was transferred to the vaccine court and (excluding a case where RFK sued Merck for fraud on their HPV vaccine) it was no longer possible to have a regular jury trial against a vaccine manufacturer.
I had a friend who worked in the vaccine court and he told me that while the process was “very fair” on the surface, the manner in which it was structured also made it nearly impossible for injured individuals to get compensation. This is because the rules of the court stipulate there has to be a scientific basis for the injury, and most vaccine injuries are censored from scientific publication
This once again circles back to why it is so problematic vaccine manufacturers are allowed to conceal adverse events from their clinical research trials, something the COVID-19 clinical trials have finally brought to light. This is also why certain injuries (such as Guillain-Barré from flu shots) make up a disproportionate number of compensated vaccine injuries, while other common ones (i.e. autism) are almost never compensated. Like many health care workers, the vaccine court also suffers from medical blindness and it too can only see specific injuries.
The issues with the National Vaccine Court have not improved, and building upon these failures, an even worse situation arose for COVID-19 where injured individuals could not sue Pfizer, Moderna or J&J and rather had to go through an even worse vaccine court, the Countermeasures Injury Compensation Program (CICP). Despite hundreds of thousands of severe injuries that have occurred from the experimental vaccinations and thousands of claims being filed to the CICP, I do not yet know of a single case that has received compensation for a vaccine injury. Per my understanding, the reason why Pfizer has avoided getting an FDA approval for the vaccine they distribute within the United States (there is no FDA approved COVID vaccine you can get in the USA) is so their product remains under an Emergency Use Authorization and therefore must be litigated within the CICP.
From asking my readers, a similar situation that prevents all compensation for vaccine injuries appears to have occurred in many European countries. It is very possible this entire situation resulted from the obscene contracts Pfizer (and possibly others) required each national government to sign (the contracts absolved Pfizer of all liability) in order to receive the vaccinations.
When the 1986 act was passed, part of the agreed compromise for enacting the program was that the federal government would conduct a study to assess the safety of vaccinations and develop an effective system for monitoring adverse reactions to vaccinations (VAERS). ICAN in partnership with RFK junior recently succeeded in a lawsuit that demonstrated the HSS had failed to ever study vaccinations for safety and produce the reports they were required by law to produce. This is a common bureaucratic tactic and likely means the HSS had no intention of doing this when they agreed to it so the 1986 act could become law.
Likewise, despite the fact that approximately 1% of adverse reactions associated with vaccination are reported to VAERS, very few people know that providers are legally required to report these adverse reactions to VAERS. This in fact is admitted on the Department of Health and Human Service’s website.
While health care providers are regularly trained and tested on a wide range of health care laws, I have never seen VAERS mentioned in a medical school curriculum, in a hospital training module, in a study materials for a board examination, or tested on any medical board examination. As a result (especially prior to COVID), few health care providers were aware VAERS (or FAERS) existed, and fewer still were aware that they are legally required to report vaccine injuries to it.
This would be immensely simple to fix, for example by having it be a topic that is tested on board examinations or having a state attorney general prosecute a few health care facilities for failing to report to VAERS, but as there is a vested interest in creating the perception vaccines are “safe and effective” this has never been done and widespread ignorance of VAERS continues to persist. Additionally, the administrative burden of reporting vaccine injuries would likely result in doctors prescribing less vaccinations, which would likewise be unacceptable for the pharmaceutical industry.
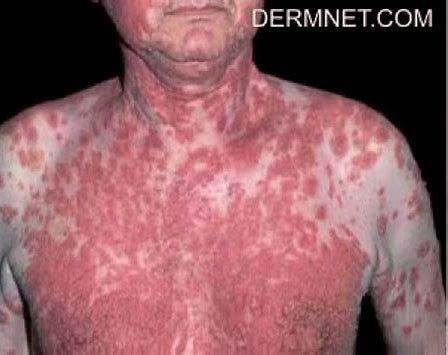
2. A colleague had a patient who developed pemphigus (an example is pictured below) after he was prescribed Lasix by his nephrologist. As my colleague would face significant legal repercussions for suggesting to his patient to stop taking Lasix, he instead gave the patient literature that stated pemphigus was a known adverse reaction to Lasix and suggested he discuss it with his nephrologist.
The patient then went to his nephrologist, who instead of discontinuing the Lasix (there are alternatives that would be less likely to create the reaction but still do what was needed), told the patient to discuss the issue with a dermatologist. The patient’s health declined and he eventually died. My colleague found this experience immensely frustrating but said it was a common experience when trying to advise specialists to consider adverse reactions from medications they prescribed.
Emotional Intelligence:
Many individuals who have had bad experiences with the medical system are left with a very poor impression of the quality of the individuals who become physicians. I deeply sympathize with this perception. However, from having interacted with many friends, associates, patients, medical students, and physicians, I believe that most individuals who are admitted to medical school are of a high caliber and it would be quite difficult to recruit better people to become our future doctors.
My uncle (who has repeatedly seen the dark side of humanity) once said to me:
”You know, AMWD, if there’s one thing I hate about the world, it’s people, and you know, if there’s one thing I love about the world, it’s people.”
Our society is largely based around conferring a mythical status to doctors, but the reality is most of them are flawed human beings just like you and me (this is something you see on a regular basis when you work with them), and the more you can interact with doctors on a human level rather than through the artificial separate ideal the society conditions us to follow, the more success you will have as a patient seeing a doctor. Just like you, doctors often have to go through very traumatic and difficult experiences at work, but at the same time they are expected to never show it and instead remain stoic and composed throughout their workday.
In the series, I have emphasized that the nature of medical training makes it very difficult for individuals to work outside of the box that Western medicine creates. However, there is however a second issue I never examined: the nature of intelligence.
Something not commonly recognized is that there are many different forms of intelligence. In our current society we value intellectual intelligence and place minimal value on the other forms of intelligence (which can sometimes be analogized to having a friend who is very smart but often times “just doesn’t get it”). Historically, this is an abnormality, as in many previous societies, other forms of intelligence (i.e. physical intelligence or emotional intelligence) were prioritized.
I follow the beliefs of certain spiritual systems which argue that an equal development of each form of intelligence rather than excessive development of one form of intelligence is ideal, and that frequently (due to the interconnectedness of the body mind and spirit), the best way to further develop one form of intelligence is to instead to work on a different form of intelligence. Due to the structure of the body mind and spirit, when someone has a high aptitude for one form of intelligence, in most cases, unless they make a large effort to train their other forms of intelligence, there will be a reciprocal deficit in their other forms of intelligence.
This is important, because typically the areas where you are underdeveloped will undermine the rest of your life, and this is particularly true for individuals with high intellectual intelligence who lead dysfunctional lives due to their deficits in their other forms of intelligence. Fields like medicine require a very high degree of intellectual intelligence, and for that reason will often attract individuals who do not have high intelligence in other areas such as emotional intelligence. When I discussed this entire issue with one of my teachers, he stated “I don’t see why you are getting so upset about this, being smart has nothing to do with your ability to resist mind control.”
Modern Education
The modern education system trains people to “think” in a very mentally lazy way. Rather than letting your mind expand to understand a complex and confusing subject (which is often punished in academia), you are expected to search your mind for an algorithmic model you have learned, which can then be applied to understanding the subject in front of you. As discussed in part 2 of this series, there are merits to this approach, but in many other ways, especially when working with complex human beings, it also has serious shortcomings. Additionally, this tendency to default to simplistic algorithmic models is especially common during periods of stress, which the entire medical system continually creates for those who train and work within it.
I frequently debate or argue with skeptics, and in the past I had significant success doing so in large online forums. The primary reason I have spent so much time debating these topics was not to win (this focus seemed like nothing more than an energy sink), but rather has been for the purpose of understanding how “skeptics” think. In turn, I have found many of the ways they argue are in fact predefined, and I can normally tell how they will respond to something that is said, because there is a finite set of algorithms individuals are taught in school for dismissing challenges to scientific dogma.
At this point in time, I am sure you have all had the experience of talking to “smart” and “well-educated” people who won’t listen to what you are saying and will instead micro-focus on some irrelevant detail to dismiss your argument and not consider the points you are raising (which is arguably another form of gaslighting). Before you understand why people think like this, one of the most curious things about it is that the “smarter” people are, the more likely they are to behave like this.
This creates the odd situation where “uneducated” individuals viewed as intellectually inferior by society (ie. farmers) are often significantly more aware and able to grasp complexity than the “experts” we are taught to delegate authority to. In this vein, while I’ve made a herculean effort to be as knowledgeable as I can, I always listen to what my patients tell me, and every day I learn very useful things I likely would have never found out otherwise.
One of the best examples I have seen of this principle were a pair of psychology studies that found more intelligent individuals were more likely to demonstrate cognitive biases and incorrect reasoning. For those that have the time to read it (the author has many other excellent publications), it provides excellent insight on this topic and can be found here.
In summary, I believe the physician tendency towards cognitive blind spots arises from an educational system that emphasizes the form of thinking where you rapidly select and then apply an algorithmic model to simplify any complex situation you encounter. Those who excel at this process tend to be promoted within academia, and amongst other things have the best transcripts for eligibility towards medical school.
When you have other forms of intelligence developed (such as emotional intelligence, intuitive intelligence or wisdom), you are much less susceptible to predefined thought patterns. Depending on how you look at it, around 5-10% percent of the population (that entire topic is a long article in of itself) are resistant to this common form of mind control and typically are the “problematic” members of society that eventually destroy existing paradigms.
How to Be Heard by Skeptics:
If you are really good and debating a contentious topic in person (online it is almost impossible to succeed), it is possible to “win” and get someone to admit your perspective is correct. However, in the vast majority of cases, if you use force to challenge someone’s ingrained beliefs (which tend to become more ingrained with increasing levels of education), regardless of how correct you think you are, it is an exercise in futility to change the person’s beliefs and you will just be butting egos against their programmed psychological defense mechanisms.
The primary reason why I devoted a section of this series to “politics,“ was because the issue I’m describing is identical to what you encounter in a polarized political issue. Regardless of the specific point, once an issue has become politicized, people who identify with the political party of the issue will be unwilling to look at arguments which challenge their viewpoints, regardless of the merits of the argument.
For example, individuals frequently find when they raise important points, rather than those points being listened to, they are labeled as a “racist” (or something similar) and this labeling becomes the basis for evaluating and dismissing their argument. I would argue that this behavior is simply an elementary example of the mental laziness individuals are trained to follow by the educational system.
When you engage these types of people, the first step you must take is to avoid appearing like someone they can put a bad label on in order to commit an ad hominem attack and thereby dismiss your point. In the case of having a doctor recognize an iatrogenic injury, this means you must be perceived as a genuine, knowledgeable, and sane patient who respects their doctor. If you are unable to create this perception of yourself, it is quite likely the doctor will view you through a negative label and use that to dismiss the evidence of your injury.
It is very common that doctors see patients who are in emotional distress or who have mental illness. As doctors are routinely taught to dismiss iatrogenic injuries as being psychosomatic diseases, it is important to not have a demeanor which could be interpreted as you being mentally imbalanced and thus responsible for your own disease. This can be very challenging given how maddening and frustrating the entire process is, but you nonetheless must do your best to avoid being categorized as another psychiatric patient.
Before seeing the doctor, make sure you are reasonably presentable (individuals with mental illness frequently are disheveled or neglect basic details such as having matching colored socks). When you see the doctor, stick to the facts of your illness, and do not broach broader political topics (ie. that the FDA is corrupt), as this will frequently place the conspiracy theorist label on you, which once again will be used to dismiss your reported symptoms.
It is fine to cry (provided you do not emotionally destabilize and start bawling), when describing the health complications you’re experiencing, as this will make the doctor empathetic towards your circumstances and make you appear genuine. However, outside of this, you want to remain emotionally composed. Do not get angry or direct hateful language towards the doctor (rather in a calm voice state that the process has been immensely difficult and frustrating for you).
When you directly challenge or attack someone, they will typically be unwilling to compromise on their position (which is one way to sum up the current political discourse). However, if you convey your message in a non-confrontational manner, and also make it clear you are willing to listen to and seriously consider the other party’s point, it creates the space for an open dialogue to happen and for your point to be heard.
This approach is especially effective if you can make the other party feel you are creating a safe space for them to express a viewpoint that is frowned upon (which is often the case within the medical field for acknowledging iatrogenic injuries). This has been critical for me to establish before red-pilling other doctors. As much as possible to create this open space, you should give the doctor the benefit of the doubt when you speak with them.
Frequently, the best you can hope for is to plant a seed that will later sprout. It is my belief that many of the physicians who are now acknowledging side effects from the COVID vaccines are doing so because they had patients who clearly made the case to them that they had been vaccine injured. Those seeds in turn were able to sprout in the doctor’s mind because the doctor had subsequent experiences which made them think back to and remember the patients they saw who effectively made the case they had likely been vaccine injured.
As much as possible, you want to avoid directly challenging the physician’s belief structure. Nonetheless you will frequently have to because your message was not listened to. While it is your personal call on if you want to take this approach, I think it is advisable to come off as someone who believes in the medical system, believes in their doctor, and just happened to have a significant adverse reaction to a pharmaceutical drug they never imagined could happen (as otherwise the “nocebo” label can be put onto you to dismiss your symptoms).
Similarly, when you describe the problems you have experienced, you should not direct any blame or animosity towards others. If you do this with the doctor, they will often get defensive and not listen to you.
In addition to coming from an appropriate emotional space, it is also important to have some credibility when your alleged medical injuries are disputed. If you have scientific credentials, try to bring them up when you are asked about your employment history (ideally in a manner which makes you sound credible, but not in a manner that comes off as someone who is trying to tell everyone they have a PhD or got a high score on the SAT).
With your specific symptoms, bring any and all documentation you can provide to describe what happened to you. In most cases this will equate to a record of you receiving the medical procedure or pharmaceutical in question, and any medical documentation corroborating the occurrence of the adverse events you are describing. If you have a family history of anything similar occurring, this is good to mention (doctors are often more prone to believing something if it is in the family history, as this is something every medical student is trained to assess). It is also a good idea to demonstrate that you have trying to find another explanation for your illness, and to the best of your ability have ruled out all other potential causes of your debilitating symptoms.
If the doctor is still resistant to considering that the pharmaceutical could have caused the adverse events, it is important to become firm in your position while remaining accepting of the doctor’s perspective. At this point, you want to mention that the same thing later happened to people you know (and state this is what made you begin to consider a potential association). After that, you want to be able to cite any published literature that supports the occurrence of the adverse event you are experiencing.
When taking this approach, it is important to avoid “controversial“ literature, as doing so may make the doctor fixate on the poor credibility of your sources being the actual explanation for your illness. The ideal literature is something published by a prestigious medical journal, admitted adverse reactions (such as that found with the pharmaceutical’s label or on drugs.com), and statements from authoritative sources such as the FDA and CDC. Unideal sources are anonymous online reports of the same symptom on the Internet (regardless of the fact these are often very helpful and have taught me a great deal) and articles written by dissident physicians who have been unfairly labeled as “quacks“ by the medical establishment.
My Eyes Glaze Over (MEGO)
From a reader, I discover the acronym MEGO, which previously was used to describe the experience many patients with fibromyalgia and chronic fatigue (common conditions conventional doctors cannot address) have when they describe their problem to a doctor. I believe you can classify MEGO as both a form of mental laziness (as the doctor does not want to create the mental strain consider the possibility that a disease outside their diagnostic box had occurred) and as a form of dissociative hypnosis (discussed in part 3 of this series).
When you see disassociation is occurring, it is important to bring the doctor back to the present and communicate directly with them. If you cannot bring them to the present, it is very likely their recollection of your interaction will be one where you are simply a replica of the archetype they have affixed to patients with your condition.
Provided you can recognize when the doctor has mentally disassociated from their interaction with you, many of the steps I described so far can help bring them back into the present with you. Creating a space where the doctor feels safe to explore a taboo topic like iatrogenesis with you and having some type of emotional engagement or connection with the doctor is often very helpful to have them be present with you. Maintaining eye contact (provided it’s not overdone), empathizing with the difficulty of the doctors position, and non-verbally responding to their non-verbal language can often be very helpful as well.
The Constraints of Medicine:
When you see a doctor for a medical injury, you should be clear with yourself what your objective is. For the majority of medical injuries, it is not possible to receive financial compensation. The primary times you can are when it’s clear (from the perspective of those who ardently support the medical system) the doctor screwed up and seriously injured you, or when a class action lawsuit is conducted against a medical facility, pharmaceutical company or medical device manufacturer.
While you cannot receive direct compensation for an injury, you will often require formal medical documentation that the injury occurred. This is typically either to be excused from work, for your family to believe you, or for when you are filing for disability. On that note, having assisted many patients navigate the disability process, I believe it is typically to your benefit to avoid going on disability unless you absolutely have to. I have also observed that over half of those seeking disability that I have met, were individuals who were failed by the medical system and would have never become disabled had the medical system functioned properly.
In medicine there is a term called “malingering,“ which is used to describe patients who are faking an illness so that they can get some type of financial reward (most frequently this comes up either for individuals faking disability or those seeking opioid medications for pain). This is another label you do not want to have applied to you, because it will be used to dismiss the legitimacy of your medical injury.
The more genuine you appear, the more documentation you have to support the occurrence of your medical injury and the less there is a reason to suspect that you are seeking to financially gain from the acknowledgment of an adverse injury, the better a chance you have to not be flagged as a malingerer. Additionally, if the topic comes up naturally, I believe to further dispel the notion you are malingering, it is helpful to inform the physician that no one has received financial compensation for a Covid vaccine injury, and that you also do not expect to be able to do anything about the legal immunity that has been given to the manufacturers.
As it is unlikely that you will ever receive financial compensation for a pharmaceutical injury, you should understand and focus upon what you can benefit from when seeing a doctor. In many cases, this will either be to get medical care for your injury, or to open the doctor’s eyes so future patients are protected from receiving the medical injury you had. Many patients will also seek to have a doctor provide a validation of what they happened to them, but I suspect most of my subscribers do not belong to the demographic that psychologically needs a physician to affirm the existence of an iatrogenic injury.
I have tried to discuss some of the strategies for opening a doctor’s eyes to the occurrence of a pharmaceutical injury. Unfortunately, while recognition of an iatrogenic injury often can be accomplished, pharmaceutical injuries tend to respond poorly to additional pharmaceutical management, and in most cases “more pharmaceuticals” is how doctors treat pharmaceutical injuries. The other common piece of advice, stress reduction, in many cases is mentioned to gaslight the patient, but can also partially improve your symptoms if you have a high baseline level of stress.
Navigating the Constraints of Medicine:
Up to this point, I have focused upon what you can do to create a positive impression with the doctor you see so that they will provide you with the best possible care for your medical injury. That said, there are also three important things you can do on your end independent of the interpersonal interactions which will significantly increase the likelihood of a successful medical experience.
First, you need to find the right doctor to work with. Typically, the best way to do this is through word of mouth referrals (provided it does not come from that friend who is psychologically invested in telling everyone they have the best doctors ever). All the people I know who are really good and can perform miracles for their patients do not advertise publicly and have built a full practice entirely through word of mouth. The alternative medical field is somewhat of a Wild West, and it is very common for me to encounter patients who spend a lot of money (sometimes in the six figures range) to see alternative healthcare providers who are ultimately unable to improve their illness.
As it is often impossible to get the word of mouth referral you need, I can only suggest two rules which may help. My own belief is that the more aggressively a healthcare provider markets themselves or tries to create a clinic experience that “pampers the patient,“ the less effective the healthcare provider is at actually addressing the issues of their patients. It is also important to trust your intuition and avoid doctors who give you a bad feeling (keeping in mind that in certain fields such as surgery, the best surgeons often have a terrible bedside manner).
Second, as you often will only be able to see a conventional practitioner who has a very limited appointment time for you, you want to make the best of the time that you have. I believe providing a well-structured and printed summary of everything a doctor would ask you during a visit (including all the key information pertaining to your medical injury) makes it easier for the doctor to understand what happened to you, and makes a significant amount of time be available for you to discuss your medical circumstances. If this is something you elect to do, look up online what goes into a history and physical (H&P), and make sure to include in your written summary everything that is asked for within the history section of an H&P.
Lastly, due to some nefarious laws passed by Richard Pan in California (discussed here), physicians there can lose their licenses for writing any vaccination exemption that does not adhere to existing guidelines for ineligibility to vaccination. Since existing guidelines state there are effectively no contraindications to vaccination, this creates a situation where doctors cannot write exemptions, even for patients who were nearly killed immediately after receiving a vaccination (I periodically hear examples of this). In certain places, writing an exemption for any reason can cost the doctor their license or job, and California’s medical board has made a point to make very public examples out of doctors who wrote a tiny number of very reasonable vaccine exemptions.
Fortunately, there is a very simple solution to this problem. If you need a medical exemption written, and you have a good case for one, see a doctor who lives in a very red state, as their medical boards will be unlikely to prosecute the doctor for any reasonable medical exemptions. It is also important to make sure they do not have a separate license in a state like California, as this puts them under the jurisdiction of that medical board, even if they do not practice within it (and penalties from one medical board can transfer over to other medical boards).
Conclusion:
When individuals are trapped in a place of myopic (close minded) algorithmic thinking, the more you engage in open communication and genuinely speak from the heart, the more likely the other person is to tap into their other forms of intelligence and break out of the myopic bubble their intellectual programming has trapped them within.
Two of the most successful activists in history are Mahatma Gandhi, and Martin Luther King (who based much of his actions off of Ghandi). Arguably, you could also include Jesus Christ in this group. The strategy of these activists recognized that if they attempted to fight an oppressive government or rival political tribe with force, all this would do would be to further strengthen the government and increase the polarization and division within the country. If you instead focused on forming a common bond, with everyone en masse refusing to comply but without directly attacking the other side, many of the oppressive hierarchies that are maintained with force and division implode upon themselves.
Fundamentally, I believe this approach works because administering force to a dysfunctional system is more likely to reinforce its dysfunction than to eliminate it. It is important to be firm, but once you cross the line to where you are attempting to apply force to a non-cooperative healthcare worker in order to change their minds, like everything in politics, the most likely response is for healthcare worker to increase their opposition towards you. If you’re really good, it is possible to win with force, but in most cases if your goal is to be successful, I highly advise against this approach.
At the same time, within our current political system, there are certain people who have gone off the deep end and have no intention of ever compromising or listening to an opposing view point. I believe whenever it is possible, you should always give everyone the benefit of the doubt. However, with these specific individuals it is a lost cause to try to have open communication with them; rather it is best to be forceful and unrelenting in your position, as these lost souls typically are cowardly and will immediately back down when they are met with strength.
Lastly, this was by far the hardest part of the series to write, which is why I did it last and after thinking it over for a few weeks. I know there is significant room for improvement in this piece. Since the advice contained within here will likely affect many people who read this article and seek physician help for a medical injury, I once again humbly request any healthcare providers reading this too give suggestions for improving the likelihood of an iatrogenic injury being recognized by a healthcare provider. I know this was a long series, and I appreciate you taking the time to examine my attempt to elucidate this immensely complex subject and share it with others.
Postscript: the most common response I have received to this article is a general disgust it is necessary to communicate with doctors in this fashion. There is a huge variation in the doctors you will see; and many are wonderful. The advice here was meant to be applicable for the more difficult doctors in order to give you the highest likelihood of success with what you need to get from the visit. Many of you are justifiably angry at the medical system, but if you project that onto the individual doctor you see, it decreases the likelihood you will get what you need.


My first thought after reading this is to avoid the whole issue by never going to a doctor again unless I'm in a car accident or break my leg. Disgusting sucking up to a person abusing his or her power.
I so appreciate your methodical navigation of today's iatrogenic hell! Having been raised with Stanford trained doctors and engineers but also a more brilliant mother from the school of Price Pottenger, the intellectual tyranny of allopathic medicine and sidestepping it has been my life's work. My childhood was full of broken dishes and fighting, fracturing my family. I escaped to Alaska and raised four sons who never saw a doctor. So much can be summed up in my favorite joke - " What's the difference between God and a doctor? God doesn't think he's a doctor".